Thanks to Invisalign, patients no longer have to endure months or years of wearing metal brackets, dealing with dietary restrictions, and scheduling monthly adjustment appointments. That said, there are some treatment guidelines you need to follow, particularly if you want to avoid frustrating delays. With this in mind, keep reading to learn a few important dos and don’ts with Invisalign!
(more…)Dr. Richard S. Tutin's Blog
Makeover Musings: How Long Does It Take to Enhance My Smile?
February 6, 2025
If you’re frustrated by dental flaws, you’re not alone. Imperfections that detract from your looks can leave you feeling so self-conscious about being judged by others that you avoid social activities. Fortunately, your dentist can provide one or several cosmetic services to help!
Some patients only require minor adjustments to boost their confidence, like removing stubborn stains with a professional whitening procedure, for example. Others have more severe aesthetic concerns requiring more involved treatments to address, like a complete smile makeover. If you’re considering this option but are unsure how long it usually takes, continue reading to learn more!
(more…)Minimally Invasive Dental Cosmetics That Can Enhance Your Smile
December 2, 2024
Dentists do great work, but if all dental treatments could be short and sweet, then most patients would probably choose that option!
When it comes to cosmetic dentistry, though, that utopia is more or less a reality. Many dental cosmetics are conservative, minimally invasive, and thanks to modern technology, faster and more convenient than ever. If this piques your interest, keep reading for a list of simple yet effective smile-enhancing options.
(more…)Dental Crown Recovery 101: Everything You Need to Know
October 15, 2024
Are you scheduled for an upcoming dental crown procedure? If it’s your first time, you may have questions about what happens afterward. Recovering from dental crown placement usually takes just a few days, during which your body heals from minor irritation and inflammation. Read on to learn what to expect and some helpful tips to ensure a smooth recovery.
(more…)A Close Shave: How Much Enamel Is Removed Before Placing Porcelain Veneers?
August 13, 2024
If you’ve watched any movies or television programs over the past few decades, you have almost certainly seen the amazing results of porcelain veneers without even noticing them. Actors and movie personalities often use these versatile cosmetic dental appliances to beautify their smiles by concealing flaws like gaps, chips, cracks, or stains or even reshaping teeth entirely. However, placing veneers requires the irreversible removal of a small amount of enamel for the appliances to fit properly. Here’s a guide to how much enamel must be removed to place porcelain veneers.
(more…)Turning Up the Brightness: Why Summer is Ideal for Teeth Whitening
June 14, 2024
Everyone knows that summer is the time for sunshine, vacations, and social gatherings. But did you also know that it’s also the perfect season to brighten your smile? If you’re curious how the sunniest season around could be good for teeth whitening treatments continue reading!
(more…)Restoration Retention: How Long Do Fillings Last?
April 10, 2024
If you’ve had a cavity in recent years, there’s a good chance your dentist repaired the damage with a tooth-colored filling. Unlike the amalgam metallic fillings of the past, this bio-compatible material bonds with your enamel to restore your tooth’s structure. That means your dentist doesn’t have to remove as much of your enamel to ensure that it remains in place. Plus, it can be customized to match your natural hue, so no one will notice it’s there.
It’s natural to wonder how long you can expect your restoration to last if you’ve learned that you need a filling. Continue reading to learn more about what kind of timeline to anticipate!
(more…)Helpful or Pointless: Do Adults Need Fluoride Treatments?
February 15, 2024
If you get dental care often, you likely know about fluoride treatments. These procedures apply a special varnish to a patient’s teeth. That said, you may wonder: do adults need fluoride treatments? Many people assume these sessions only work for kids. Well, you can rest easy – the fluoride varnish also helps grown-ups. Your local Framingham dentist is here to tell you why. So, read on to learn why an adult may need fluoride treatment.
(more…)3 Procedures You May Need Before Getting Dental Implants
May 4, 2023
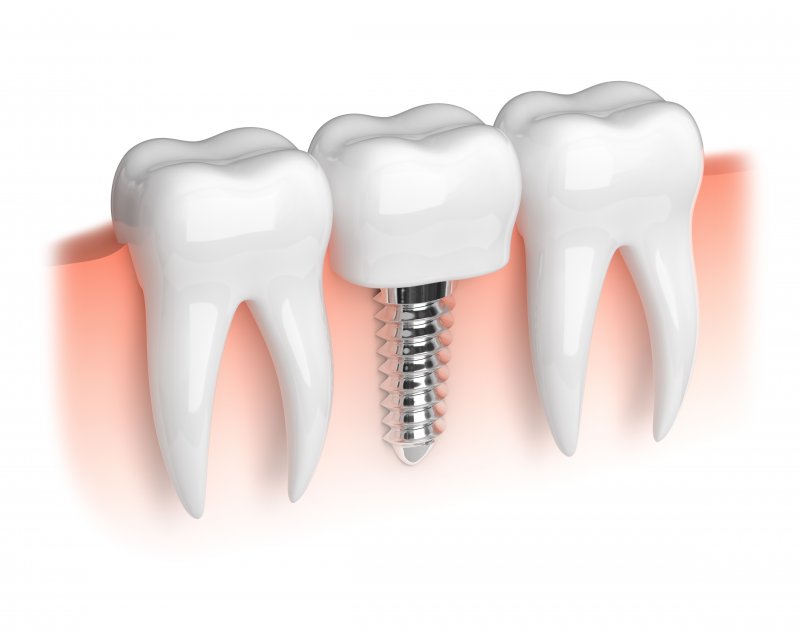
For individuals with missing teeth, dental implants serve as an excellent solution. These titanium artificial tooth roots are surgically inserted into the jawbone to provide support for replacement teeth restorations, like dental crowns. Not only do dental implants offer a natural appearance, but they can also last for decades when properly maintained. However, in certain cases, patients may require preparatory procedures to ensure the successful placement of implants. keep reading to learn about three preliminary procedures that you may need prior to receiving dental implants.
(more…)Why Dental Implants are the Pinnacle of Tooth Replacement
April 5, 2023
If you’ve been looking into replacing missing teeth for any time at all, you’ve probably heard something about how incredible dental implants are. They’re one of the top methods of tooth restoration that dentists recommend, and one of the most celebrated among patients.
But are they really all that they’re cracked up to be? If you want to know why so many people call dental implants the pinnacle of tooth replacement, here are a few good reasons.
(more…)